Foot fungus is a concern among athletes, thriving in the warm, damp environments of locker rooms, sweaty socks, and athletic footwear. Left untreated, it can lead to discomfort, odor, and even serious infections that sideline performance. Understanding how foot fungus, known as athlete’s foot, develops, and how to treat and prevent it, is key to maintaining foot health and staying active. Let’s explore the causes, risks, and effective solutions for managing athlete’s foot.
Signs and Symptoms
The following are common signs and symptoms associated with foot fungus. Recognizing these early indicators is fundamental for timely intervention and treatment:
- Persistent itching and burning sensations, particularly between the toes.
- Dry, scaly, or peeling skin on the feet.
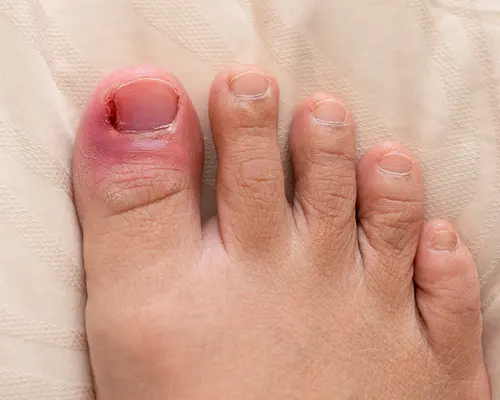
- Red, inflamed, or irritated patches of skin.
- Cracked skin, which may lead to discomfort or pain.
- Thickened, brittle, or discolored toenails when the fungus spreads to the nails.
- Foul odor emanating from affected areas.
If you observe one or more of these symptoms, seeking medical advice can help confirm the diagnosis and guide proper management strategies.
Causes and Risk Factors
Athletes face multiple risk factors that increase their likelihood of developing foot fungus. The primary factor involves spending extended periods in enclosed athletic shoes that trap moisture and heat. Human feet contain a lot of sweat glands that produce significant amounts of moisture during physical activity.
Heavy sweating during training and competition creates a damp environment that fungi need to thrive. Athletes frequently walk barefoot in community showers, locker rooms, saunas, and pool areas where contaminated surfaces harbor fungal spores. Sharing equipment, towels, mats, and facilities with other athletes increases the risk of exposure to infected materials.
Treatment Options
Several treatment approaches effectively address fungal foot infections. Over-the-counter antifungal creams, sprays, and powders provide the first line of defense against mild infections. These topical medications contain active ingredients that directly target fungal growth.
Apply these treatments daily to clean, dry feet, extending the application beyond the visible infection area to prevent spreading as directed. Continue treatment for at least one week after symptoms subside to make sure the infection is eliminated. Most mild cases respond well to consistent topical treatment within two to four weeks.
Severe or persistent infections require prescription medications from a healthcare provider. Prescription-strength topical treatments offer higher concentrations of antifungal compounds for stubborn infections. Oral antifungal medications may be necessary for extensive infections or cases that don’t respond to topical treatments.
Prevention
Preventing athlete’s foot requires consistent foot hygiene practices and awareness of environmental factors. Keep your feet clean and completely dry, paying special attention to areas between your toes where moisture accumulates. Wash your feet daily with soap and water, then dry them thoroughly before putting on socks and shoes.
Change socks immediately after workouts or whenever they become damp from sweat. Wear shoes with good ventilation that allow air circulation around your feet. Rotate between multiple pairs of athletic shoes, allowing each pair to dry completely between uses. Use antifungal powders or sprays in your shoes to help control moisture and prevent fungal growth.
Schedule a Foot Fungus Evaluation Today
Athletes are disproportionately affected by foot fungus due to the warm, moist conditions their feet experience during training and competition. Recognizing early symptoms and starting treatment promptly can prevent complications and reduce the risk of transmission to others. If you suspect you have athlete’s foot or experience recurring fungal infections, contact a healthcare provider and schedule a foot fungus evaluation for proper diagnosis and treatment recommendations.