Arthritis constitutes a broad spectrum of disorders affecting the musculoskeletal system, and it stands as a leading cause of disability in the United States. The condition is characterized by chronic pain and functional limitation, necessitating a multifaceted approach to clinical management. Here is more information on arthritis and the therapies available to patients:
What Is Arthritis?
Arthritis is not a single disease; it is a term for joint pain or disease. There are more than 100 different types of arthritis and related conditions, and people of all ages, sexes, and races can have them. It is a leading cause of disability in America, but early diagnosis and appropriate management can improve quality of life.
The condition typically involves inflammation or degeneration (breakdown) of your joints. These changes can cause pain when you use the joint, or they lead to stiffness that persists throughout the day. While some forms are related to wear and tear, others are autoimmune diseases where the immune system attacks healthy tissue.
What Are the Different Types?
Osteoarthritis is the most common form of arthritis and typically affects the hands, hips, and knees. It involves the breakdown of cartilage and the underlying bone, and symptoms often develop slowly and worsen over time. Patients may notice a grating sensation when using the affected joint or experience tenderness with light pressure.
Rheumatoid arthritis and psoriatic arthritis are autoimmune inflammatory types. In these conditions, the immune system mistakenly targets the joints and potentially other organs, leading to widespread inflammation. Gout is another common metabolic type caused by the accumulation of uric acid crystals in the joint, often affecting the big toe first.
What Causes Them?
The causes of arthritis vary by type. In osteoarthritis, the cartilage that cushions the ends of bones wears down over time, or an injury can precipitate the damage. This deterioration allows bones to rub directly against one another, causing friction, pain, and eventual swelling.
In autoimmune conditions such as rheumatoid arthritis, the immune system attacks the lining of the joint capsule. This lining becomes inflamed and swollen. Disease processes can eventually destroy cartilage and bone within the joint, so early intervention is key for preserving function.
What Are the Symptoms?
The most common signs of arthritis involve the joints, and these symptoms vary between individuals. Pain, stiffness, swelling, redness, and decreased range of motion are primary indicators of joint inflammation or degeneration. Symptoms may come and go or persist consistently over time. In severe cases, chronic arthritis can result in permanent joint changes.
What Are the Treatment Options?
Doctors often begin with conservative measures to manage pain and reduce inflammation. Over-the-counter painkillers help manage mild discomfort, while rest and ice packs can reduce acute swelling. Counterirritants may interfere with the transmission of pain signals from the joint.
When conservative methods are insufficient, physicians may prescribe disease-modifying antirheumatic drugs (DMARDs). These medications slow the progression of rheumatoid arthritis and help prevent permanent joint and tissue damage. Corticosteroids act quickly to control inflammation, and doctors may prescribe them for short-term use.
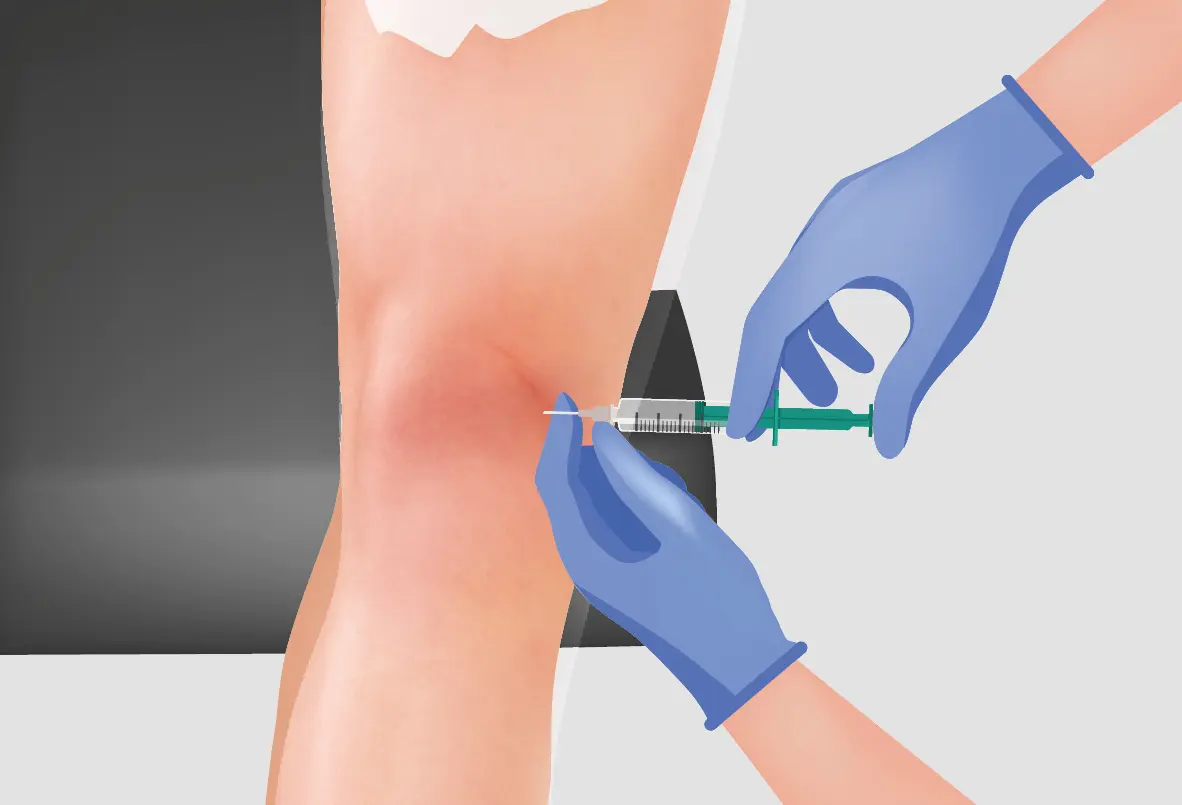
For localized relief, hyaluronic acid injections can provide lubrication directly into the joint space. This substance mimics the fluid naturally found in healthy joints, reducing friction and improving shock absorption. In cases where joint damage is severe and unresponsive to other treatments, surgical options are available.
Consult a Specialist Today
Living with arthritis requires a comprehensive management plan tailored to your specific symptoms and lifestyle. Early diagnosis and treatment are key to slowing disease progression and maintaining joint function. Schedule an appointment with a specialist to discuss which traditional or innovative therapies are right for you.