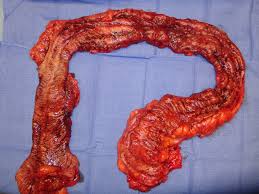
Ulcerative colitis is a chronic inflammatory bowel disease that affects the large intestine. Understanding this condition is the first step toward managing its impact on your daily life and long-term health. A definitive diagnosis, often achieved through procedures like a colonoscopy, is beneficial for developing an effective management plan with a gastroenterologist. This process provides a clear view of the colon, enabling doctors to accurately assess the extent and severity of inflammation and guide appropriate care.
Defining Ulcerative Colitis
Ulcerative colitis is a condition characterized by persistent inflammation and ulcers in the innermost lining of the colon and rectum. Unlike other inflammatory bowel diseases, it exclusively affects the large intestine in a continuous pattern starting from the rectum. The immune system mistakenly attacks the colon’s lining, resulting in inflammation and symptoms characteristic of the disease. A colonoscopy is a primary diagnostic tool, allowing physicians to directly visualize the affected tissue, confirm the diagnosis, and distinguish it from other conditions with similar symptoms.
Recognizing Key Symptoms
The symptoms of ulcerative colitis can vary in intensity and may develop gradually or appear suddenly. Some of these symptoms include:
- Individuals with this condition often experience persistent diarrhea, which may be accompanied by blood or pus.
- Abdominal pain and cramping are also common, along with a frequent and urgent need to have a bowel movement.
- Other potential symptoms include unexplained weight loss, fatigue, and fever, which can significantly affect one’s quality of life.
If you experience any of these symptoms, it’s helpful to consult a healthcare professional for proper evaluation and treatment.
Understanding Common Triggers
While the exact cause of ulcerative colitis is not fully understood, certain factors can trigger or worsen symptoms. Dietary choices are a significant factor. Specific foods may irritate the colon and lead to a flare-up. Stress and emotional distress do not cause the condition, but they can intensify symptoms for many individuals. Other potential triggers may include the use of nonsteroidal anti-inflammatory drugs (NSAIDs) and certain environmental factors. These can vary widely from person to person.
Exploring Treatment Options
Gastroenterologists treat ulcerative colitis with the primary goal of inducing and maintaining remission. Treatment plans are tailored to each individual and often combine multiple approaches. Medications play a central role in therapy, including anti-inflammatory drugs and biologic therapies that target specific components of the immune system.
Beyond medication, lifestyle and dietary changes may be recommended to help manage symptoms and prevent flare-ups. When medications are ineffective or complications occur, surgery to remove the colon may be an option. This comprehensive approach helps patients receive the most effective care for their condition.
Schedule a Colonoscopy Today
Early and accurate diagnosis is beneficial for effectively managing ulcerative colitis and preventing potential complications. By understanding the symptoms and seeking timely medical evaluation, you can play a role in your gastrointestinal health. If you are experiencing persistent digestive issues, it is helpful to consult with a GI doctor immediately to determine the cause. Schedule an appointment to discuss your symptoms and determine if a colonoscopy is the right next step for you.